|
5% of bone mass every year after the age of 50. Race: Asian and Caucasian women, especially those who are small-boned, are at highest risk.įamily history: Patients with a family history of low bone mass have a 50%-85% increased risk of developing osteoporosis.Īge: Most people (men and women) lose about. Women also often experience a loss of bone mass after menopause. Gender: Women are a higher risk because they have less bone mass than men. However there are certain risk factors that can increase the likelihood that a person will have moderate to severe loss of bone mass, including the following: Not everyone will get osteopenia or osteoporosis. Who Is at Risk for Osteopenia/Osteoporosis? For these patients, treatment is usually necessary and includes the use of medications to help increase bone mass, as well as lifestyle changes such as diet and exercise. Patients with T-scores lower than -2.5 SD are diagnosed with osteoporosis. Patients with T-scores between -1 SD and -2.5 SD are diagnosed with osteopenia and are considered at high risk for osteoporosis. T-scores can fall as low as -1 SD and still be considered healthy (see table below). The difference between the "normal young" score and the patient's score is referred to as a standard deviation (SD). What the BMD Numbers MeanĪ patient's BMD is given a T-score, which is derived by comparing it to an average score for a healthy 30-year-old of the same sex and race. The results are measured as a "score" and are compared to those of healthy individuals. This scan uses low-energy x-rays that expose patients to much less radiation than standard x-rays and can assess calcium levels in bone. While osteopenia may be diagnosed using plain radiographs, the most common method for measuring BMD (and a way to definitively diagnose osteoporosis) is through Dual Energy X-ray Absorptiometry or DEXA. Bone mineral density tests are noninvasive and painless procedures usually done on the hip, spine, wrist, finger, shin bone, or heel. It is also used to determine if a patient has osteopenia or osteoporosis. 
Osteopenia Determinationīone mineral density (BMD) is the measurement of calcium levels in bones, which can estimate the risk of bone fractures. Millions more Americans are estimated to have osteopenia (low bone mass), putting them at risk for osteoporosis. According to the National Osteoporosis Foundation, osteoporosis affects 54 million Americans, mostly women. If it progresses, osteoporosis can lead to loss of height, stooped posture, humpback, and severe pain. Many of the foods you eat contain these bone-building minerals. Osteoporosis, the "fragile bone disease," is characterized by a loss of bone mass caused by a deficiency in calcium, vitamin D, magnesium and other vitamins and minerals. The diagnostic difference between osteopenia and osteoporosis is the measure of bone mineral density. 
Osteopenia is commonly seen in people over age 50 that have lower than average bone density but do not have osteoporosis. If your T-score is –2.5 or less: you have osteoporosis, even if you haven't yet broken a bone.The diagnostic difference between osteopenia and osteoporosis is the measure of bone mineral density. 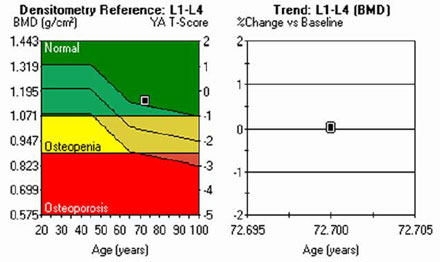
If your T-score is between –1 and –2.5: you have low bone density, known as osteopenia, but not osteoporosis.If your T-score is –1 or greater: your bone density is considered normal.The World Health Organization has established the following classification system for bone density: The DEXA scan or ultrasound will give you a number called a T-score, which represents how close you are to average peak bone density. DEXA accomplishes this with only one-tenth of the radiation exposure of a standard chest x-ray and is considered the gold standard for osteoporosis screening-though ultrasound, which uses sound waves to measure bone mineral density at the heel, shin, or finger, is also used at health fairs and in some medical offices. While this technology can measure bone density at any spot in the body, it is usually used to measure it at the lumbar spine (in the lower back), hip (a specific site in the hip near the hip joint), and femoral neck (the top of the thighbone, or femur). And it's simple: you lie on a table while a scanner passes over your body. The process is quick, taking only five minutes. For this procedure, a machine sends x-rays through bones in order to calculate bone density. Several technologies can assess bone density, but the most common is known as dual energy x-ray absorptiometry (DEXA).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
